
Table of Contents[Hide][Show]
When pet owner Risa L. told me about the benefits of Hyperbaric Oxygen Therapy for dogs, I was amazed. Her dog, Mia, suffered a life-threatening FCE (Fibrocartilagenous Embolism) stroke, but learned to walk again after receiving treatments in a hyperbaric oxygen (HBOT) chamber.
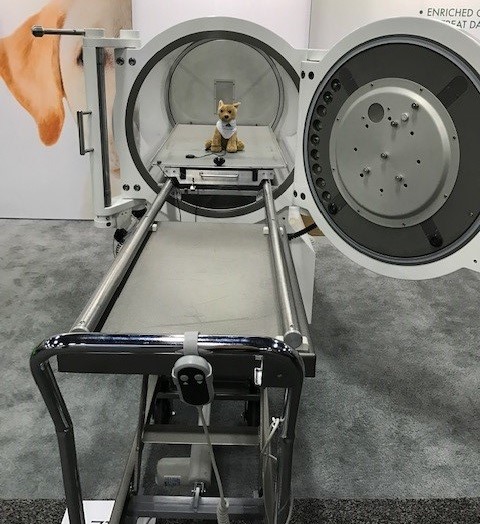
To be truthful, the idea of putting a paralyzed pet inside a pressurized cylinder, ramping up the oxygen level and then pulling them out cured and whole, seemed like science fiction to me. It seemed too good to be true.
But oxygen therapy is anything but science fiction. That’s a fact I learned during one of the most remarkable lectures I’ve ever attended.
Read more about Mia, FCE strokes and 7 Of The Most Common Spine Diseases in Dogs

Ask & Discover
Get personalized content recommendations and answers drawn from our website. Simply type your question or topic of interest, and our AI assistant will help you find relevant articles, tips, and insights. You can also have a natural conversation to explore topics in more depth.
The HBOT seminar that made me a believer

The opportunity to learn about HBOT came when Robert Hancock, DVM and founder of South Paws Veterinary Specialists in Louisiana offered a webinar about the benefits of Hyperbaric Oxygen Therapy for dogs.
Dr. Hancock was an expert in the field. His lecture was full of compassion for our pets and passion about all the ways HBOT has proven to be helpful. He spoke quickly and shared so much information that I had a hard typing all he had to say into my computer.
Sadly, Dr. Hancock passed away soon after his presentation. His passing makes the information I am sharing in this post even more important. I’m grateful I was able to take part in the webinar and learn from this special veterinarian.
How Hyperbaric Oxygen Therapy works

HBOT isn’t a new treatment. It’s been used for hundreds of years to stop deep sea divers from getting “the bends.”
Divers used to get severe joint pain, suffer from confusion and even death when they rose to the surface from the ocean floor. The cause was the nitrogen in their blood had increased while they were underwater.
Then a scientist came up with the idea of placing the divers inside an iron bell with high levels oxygen and pressure as they came up from the bottom of the ocean. It solved the problem; divers stopped getting the bends.
The same practice is used in today’s modern version of Hyperbaric Oxygen Therapy.
HBOT needs 3 components to work:
- * 100% oxygen
- * Delivered in a pressurized chamber
- * For a specific period of time
The principle is based on two laws of physics. One is Henry’s Law and the second is Boyle’s Law. Together they discovered that when a gas is dissolved in a liquid, the concentration of that gas becomes proportional to the pressure around it. (I hope that makes sense).
For instance, the normal air we breathe is 21% oxygen and 78% nitrogen. At sea level the pressure around us is 14.7 mm. And at sea level, the oxygen level in our (human) blood is 98%. This maintains normal-sized gas bubbles in our body.
When oxygen is used as a drug and increased to 100% with a higher than normal pressure around it; the gas bubbles shrink and become more concentrated. (This is a key point.)
The process turns these small bubbles in the bloodstream into high-powered healing machines. It gets oxygen into the body 4 times faster and literally speeds up the time it takes to heal.
How Dr. Hancock tested the theory

Dr. Hancock said that while he understood the theory, the surgeon in him didn’t completely believe the concept. He needed proof that HBOT would heal his patients faster. So, he eased into it by adding sessions in a Hyperbaric chamber as part of the normal treatment plan for the dogs and cats in his care.
“There was a huge improvement in the healing process of my patients,” said Dr. Hancock. “This was a big new piece of the puzzle to me.”
HBOT isn’t a silver bullet, but it is part of a total health approach.
“Soon all of the owners of my surgical patients were asking for their dogs to have a session in the chamber.”
HBOT works best when it’s used in the early stages of a disease or recovery
Veterinarians and the pets they treat are lucky. They don’t have to wait for an insurance company to approve HBOT.
So, Dr. Hancock offered the treatment readily to his patients and saw lots of dramatic improvements in dogs suffering from:
- FCE Stroke
- Head injury
- Spinal cord injuries
- IVDD – Intervertebral Disc Disease
- Wounds
- Pancreatitis
- Peritonitis
- Post-surgical recovery
Patients with orthopedic problems generally received 3-5 HBOT treatments. And dogs with neurological conditions were given 10-20 treatments.
Read more about: When Your Dog Needs An MRI, CAT Scan or Other Imaging Test

Get the Essential Guide
The Essential Guide of Products for Handicapped Dogs e-book is a labor of love for me. I wrote it to answer your most pressing questions about where to find the best products for your wheelchair dog. You’ll find products you didn’t know existed and each will improve your dog’s quality of life. Print a copy and keep it by your side.
How HBOT is changing the lives of dogs with spinal cord problems
Dr. Hancock was particularly proud of the success his patients with disc disease had after surgery. He said most of the spinal surgeries he performed were to relieve a compression on a dog’s spine. These were conditions like a ruptured or bulging disc.
But even when the surgery was successful in repairing the anatomical problem, many dogs were still unable to walk on their own. Dr. Hancock found this frustrating.
He concluded the problem was due to the constant pressure and swelling that had built up in the spine. It cut off the blood flow to the area and the cells in that part of the spine died off. So, he added HBOT to the dogs’ aftercare.
Dr. Hancock said, “Before we added HBOT, 50% of the dogs in my practice who underwent spine surgery for disc disease regained deep pain sensations (feeling in their legs).
Deep pain sensations resumed for 78% of my patients once we started using HBOT.
This is an amazing success rate if you’re the pet parent of a dog with a spinal cord problem.
At first Dr. Hancock said he didn’t fully understand why the treatment was working so well. But later he came up with two conclusions: HBOT was soaking up free radicals and turning cells on and off, as needed.
Here are other medical conditions where Hyperbaric Oxygen Therapy for animals is being tested:
- * Prevent blood clots and infections after surgery
- * Snake bites
- * Burns
- * Fractures
- * Tendonitis
- * GI problems
- * Lyme Disease
- * Anemia
- * Abscess
- * Septic arthritis
- * Carbon monoxide poisoning
- * Cyanide poisoning
- * Gangrene
- * Diabetic wounds
- * Potentially useful for recurring Urinary Tract Infections (UTIs)
Success stories from Dr. Hancock’s patients

Dr. Hancock shared two stories about his patients. The first was a 21-year-old cat who was brought to the clinic because of a severe UTI. She hadn’t responded to other treatments. After only 3 HBOT sessions, the cat finally got relief for her infection.
The second patient was a dog who came in with a severe head tilt. His owner had been told nothing further could be done for him. Dr. Hancock placed the dog in the Hyperbaric chamber for one treatment and the problem was resolved.
Hope for the future
Dr. Hancock told webinar attendees that veterinarians are leading the way in exploring new benefits of hyperbaric oxygen therapy. For instance, Israel is currently adding stem cells to HBOT.
He believed vets had better access to oxygen chambers because of their smaller size and lower price tag than the chambers for humans. He also worried it was due to a lack of interest from pharmaceutical companies that preferred clinical trials using medications.
Dr. Hancock was a visionary. I’m so grateful I had the opportunity to hear his lecture.
Have you seen the benefits of Hyperbaric Oxygen Therapy for dogs? If so, please share your story below. I’d love to know learn about your experience.





Thanks for taking time to pass along this info Sharon. We’ve had quite a few members over the years whose dogs may have benefitted from it. Did Dr. Hancock have any info specifically about cats?
Poor guy, how sad that he died so young! But he left a legacy for sure.
Hi Rene, The webinar I attended was strictly about his work with dogs. I’m glad to hear that HBOT has helped dogs with amputations. There are so many medical advances it’s hard to keep up.
Sharon, thank you so much for sharing your experience. I have been doing hyperbaric oxygen therapy for pets for over 11 years now Dr. Hancock was going to change the face of hyperbaric oxygen therapy for pets. He was a tragic loss to the industry.
Thank you for sharing
Teri, Thank you for your comment. I’m glad you are carrying on Dr. Hancock’s legacy.